|
Singh V, Manchikanti L, Helm S, Hirsch et al. “Percutaneous Lumbar laser Disc Decompression: a Systematic Review of Current Evidence." Pain physician 2009; 12:573-588.
Note: Here's another good Danish review of percutaneous laser discectomy: it has some illustrations.
Theory | Tutorial | Study | Results | Level of Evidence | Procedure Recommendation | Conclusions | My Comments | References | Retrun to Research Corner
Theory:
For the unlucky 5% of humans that suffer medium to large disc herniation-induced back pain [5], with or without associated radiating lower extremity pain (sciatica), that don't recover with conservative care, open discectomy (a.k.a. microdiscectomy) is often very successful at ameliorating the pain and dysfunction [1, 2, 3]. However, there is a subclass of herniation types that does not respond favorably to discectomy; more specifically, it is well known that small contained disc herniations respond poorly to traditional microdiscectomy, [3, 10, 51] which makes interbody fusion the obvious alternative— fusion is certainly not a panacea and has empirical success rates of only 30-40%.
Therefore, in the hunt for more effective and conservative treatment interventions for these stubborn small contained disc herniations, numerous minimally invasive techniques have arisen. The focus of this review is on one of them, which uses laser energy to vaporize some of the nucleus pulposus of the herniated disc, thereby lessening the pressure within the disc, which in turn retracts the herniation and relieves nerve root pressure as well as pressure on the nerves-infested posterior annulus. This technique is called percutaneous lumbar laser discectomy (aka: percutaneous lumbar laser disc decompression, percutaneous laser disc decompression or PLDD) [4].
Visual Tutorial on PLD:
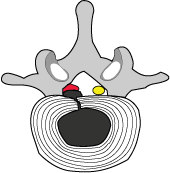 |
#1) this is our starting condition: a small contained lumbar disc herniation of the L5 disc that has compressed the right L5 nerve root (the nerve root is red with inflammation and the patient has lower back pain with pain radiating down the right lower extremity). The herniation size does not take up more than one third of the central canal size – this is a criteria for PLD |
|
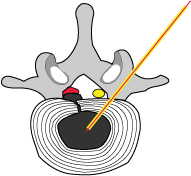
#2) a hollow needle (yellow) is obliquely inserted into the center of the intervertebral disc (i.e., the nucleus pulposus); this placement is confirmed by fluoroscopy and/or CAT scan guidance.
The red straight line represents a 0.4 mm laser fiber that has been inserted through the needle into the center of the nucleus pulposus. |
|
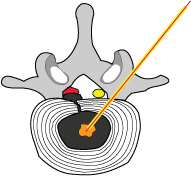
#3) laser energy is being delivered to the nucleus pulposus, which destroys the proteoglycans and aggrecan content of that tissue. This results in an immediate loss of water content as well as mass, which in turn achieves the goal of the procedure: to reduce intradiscal pressure. |
|
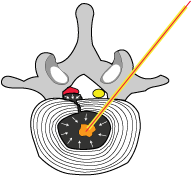
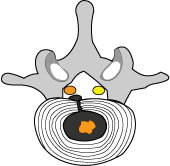
#4) the treatment is working as the nucleus is shrinking and the intradiscal pressure has been reduced. |
|
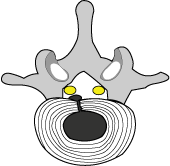
#5) the mass of the nucleus has been decreased as well as the intradiscal pressure. This has resulted in a retraction of the herniation, which in turn has relieved the pressure on the right L5 nerve root (orange and less angry). |
|
#6) the mass effect is no longer evident on the right L5 nerve root, which is healing and happy (yellow). |
Quick History:
In 1986, Ascher and Choy first used laser energy to destroy (vaporize) portions of the nucleus pulposus (proteoglycans) in order to reduce the volume of the disc, in hopes of reducing the size of a small contained disc herniation (sucks it back inside). This volume reduction in turn is thought to remove nerve root compression, as well as relieve pressure upon the pain-carrying sinuvertebral nerves of the posterolateral annulus fibrosis.
The beauty of this system was that a very smaller cannula could be used (~ 3mm) to delivery of the 400-nm laser fiber to the center of the disc, which mitigates complication rates such as discitis and epidural fibrosis. Another exciting development was the fact that most of the lasers included a fiber-optic channel so the surgeon could view just what he was vaporizing.
Initial success rates were not very promising as a number of different lasers were investigated, including the Nd-YAG, KTP, holmium, argon, and carbon dioxide lasers. However, eventually success rates dramatically climbed to as high as 88% [50] as "enthusiastic retrospective case series reports [emerged] by operating surgeons [26].
In year 2000, Gibson and Waddell [53] (two very well respected researchers) published a Cochrane review of surgery for lumbar disc prolapse, which included a review of laser discectomy's efficacy for the treatment of disc herniation. After scouring the medical research databases, the investigators could not find a single randomized controlled trial describing laser discectomy. Annoyed, this led them to opine that laser discectomy should be regarded as a research technique until better scientific evidence became available.
The Study:
In 2009, Singh et al. published the results of their systematic review with regard to the efficacy of percutaneous lumbar laser disc decompression (laser disc decompression or LDD) as a treatment intervention for symptomatic small contained disc herniations with associated radicular pain.
A thorough search of the medical literature and paper bibliographies was performed in order to find all articles written on this subject. Next, all of the studies were rated for scientific quality by the application of the methodological quality assessment tool from the Agency for Healthcare Research and Quality (AHRQ) [17]. Final recommendations were made in accord with the criteria established by Guyatt et al [46].
With regard to outcome measures, the researchers were looking at pain relief as the primary outcome measure, with functional improvement as a secondary outcome. In those regards, in order to have a "successful outcome," the patient had to achieve 50% or more relief of pain and have a 40% or more decrease in disability scores – these levels of success have been studied, substantiated and reported on in multiple publications [13-15].
Of the 33 articles that were located in the literature (there were no randomized controlled trials), methodological quality assessment eliminated all but 10 studies, which all scored above 50 on the AHRQ's methodologic quality assessment criteria for evidence synthesis. Therefore, this review looked at the results from 2447 patients.
Results:
Based on our definition of success, 72% of all patients achieved a 50% or greater reduction in pain at follow-up. The range was between 56% and 87%.
The functional outcome was assessed prospectively via the Oswestry Disability Index. Again, in order to have a "successful outcome," patients had to improve a minimum of 50% at follow-up. Because of heterogeneity regarding the functional improvement, all studies could not be compared. One of the larger studies [64], however, which consisted of 576 patients, used Oswestry scores for they are functional assessment. The functional result of that study was that 52% of the patients demonstrated an Oswestry improvement of 50% or greater past the three-year time point (the average post surgical follow-up was 5.3 years). An additional 21% also had improvement – just not as high as 50% improvement—at follow-up. That would mean that 27% of the patients failed to have any functional improvement.
In another quality observational study [52], 63 patients underwent PLDD for small contained disc herniation; 61 were available at two-year follow-up. At that time, 72% achieved a 50% or greater drop of their radicular pain (radiating leg pain), while only 54% achieved a 50% or greater dropped in their low back pain. 59% of the patients return to work by the fourth week following surgery. These authors also compared pain relief (on VAS) of their cohort to a group of patients who had undergone open discectomy. The results indicated that 85% of the patients had good to excellent pain relief following open discectomy, whereas only 66% of the patients with laser discectomy showed good to excellent results.
Level of Evidence:
The indicated level of evidence supporting PLDD as a treatment intervention for symptomatic lumbar contained disc herniation based on the USPSTF criteria (45) is Level II-2 for short and long-term relief.

Procedure Recommendation:
The recommendations for PLDD based on Guyatt et al’s criteria (46) is 1C / Strong Recommendation.

Conclusions:
The authors of this study had several worthwhile conclusions to put forth in my review:
#1) with regard to the functional success of PLDD, this intervention "provides an initially gratifying result, but the result deteriorates over a period of time,” which occurred during the second and third year.
#2) the systematic review indicated Level II-2 evidence for percutaneous lumbar laser disc decompression with 1C/Strong recommendation.
Comments:
One thing I've noticed through my massive review of the literature over these past few weeks, is that many researchers seem to take issue with Gibson and Waddells’ pooh-poohing all of these minimally invasive procedures. More specifically, the duo [5] recently concluded that the clinical outcomes following laser discectomy are at best fair and certainly worse than microdiscectomy. However, microdiscectomy actually does very poorly with regard to contained herniations [1, 3], much worse than the average relief of pain scores and functional disability that was demonstrated in this study. More specifically, Carragee [3] stated that patients with the contained disc herniation measuring 6 mm or less had only a 24% success rate after microdiscectomy. So, perhaps PLDD would have been a better treatment option for these patients.
Therefore, I wholeheartedly agree with the authors of this systematic review when they say, "Laser Disc decompression may provide appropriate relief on properly selected patients with contained disc herniations."
REFERENCES:
1) Dewing CB, et al. "the outcome of lumbar microdiscectomy in a young, active population: correlation by herniation type and level." Spine 2008; 33:33-38.
2) Gibson JNA, Waddell G. "surgical interventions for lumbar disc prolapse." Cochrane Database Syst Rev 2009; 1:CD001350.
3) Carragee EJ, et al "Clinical outcomes after lumbar discectomy for sciatica: The effects of fragment types and annular competence" J Bone Joint Surg Am - 2003; 85(1):102-108.
4) Schenk B, et al (2006) Percutaneous Laser Discectomy: A Review of the Literature. AJNR; January 2006: 27; 232-235.
5) Gibson JNA, Waddell G. “surgical interventions of lumbar disc prolapse." Cochrane Database Syst Rev 2009; (1): CD001350.
10) Carragee EJ, et al. "Can MR scanning in patients with sciatica predict failure of open limited discectomy? Proceedings of the international Society for the study of lumbar spine (ISSLS) Scotland, June 2001.
13) Manchikanti L, Hirsch JA, et al. “evidence-based medicine, systematic review, and guidelines in interventional pain management: part 2: randomized controlled trials. Pain physician 2008; 11:713-775.
14) Manchikanti L, et al. "evidence-based medicine, systematic reviews, and guidelines in interventional pain management: part 3: systematic reviews and meta-analysis of randomized controlled trials. Pain physician 2009; 12:35-72.
15) Manchikanti L, et al. "evidence-based medicine, systematic reviews, and guidelines in interventional pain management: part four: observational studies. Pain physician 2009; 12:73 – 108.
17) West S, et al. “system to rate the strength of scientific evidence, evidence report, technology assessment number 47. AHRQ publication number 02-E016. Rockville, MD: agency for healthcare research and quality, 2002. www.thecre.com/pdf/ahrq-system-strength.pdf
26) Singh V, Derby R. "Percutaneous Lumbar Disc Decompression." Pain physician 2006; 9:139-146.
46) Guyatt G et al. “Grading Strength of Recommendations and Quality of Evidence and Clinical Guidelines. Report from an American College of Chest Physicians Task Force." Chest 2006; 129:174-181.
50) Ahn Y, Lee Sh, et al. "Factors predicting excellent outcome for percutaneous cervical discectomy: analysis of 111 consecutive cases. Neuroradiology 2004; 46:378-384.
51) Dewing CB, et al. "the outcome of lumbar microdiscectomy in a young, active population: correlation by herniation type and level." Spine 2008; 33:33-38.
52) Bosacco et al. “Functional Results of Percutaneous Laser Discectomy." Am J Orthop 1996; 25:825-828.
53) Gibson JN, Grant IC, Waddell G. "Surgery for lumbar prolapse." Cochrane Database syst Rev 2000; (3):CD001350.
64) Knight M, Goswami A. “lumbar percutaneous KTP532 wavelength laser disc decompression and disc ablation in the management of discogenic pain." J Clin Laser Med Surg 2000; 20:9-13.
Top | Research Corner | Home
Copyright © 2002 – 2012 by Dr. Douglas M. Gillard DC
|

